What is Stage II melanoma?


Dr. Jason Luke: I can provide a quick summary. This can be a little challenging to grasp, so I will then delve into the details about how the two factors of depth (thickness) and ulceration status (whether the skin over the melanoma is intact or not) impact staging. A detailed discussion of staging is included in the Staging Overview sidebar.
Stage II melanoma is generally thicker than Stage I melanoma. It is a melanoma that is local, meaning it has not spread either regionally (to the nearest lymph nodes or the region between the original melanoma and the regional lymph nodes) or distally (to other parts of the body beyond the regional lymph nodes). Stage II melanomas are either more than 1 mm but less than 2 mm in depth and ulcerated or they are deeper (greater than 2 mm in depth), regardless of ulceration status.
Let’s look specifically at depth and ulceration status.
Depth (thickness) of the tumor means how deep within the skin did the melanoma grow? This is a little bit different than some other kinds of cancers, where the main concern is how big it is. It can be the case that a melanoma on the skin looks quite large with a splotchy appearance but in reality is not a deep lesion. So, the deeper it goes into the skin, the worse it is.
Ulceration means if the skin covering your melanoma was intact or not, as we already have said. On visual examination, ulceration typically means the melanoma was bleeding or looked crusty. This is also a finding under the microscope that we look for and means that we might be able to see changes in the cells and skin tissue. Ulcerated is worse than non-ulcerated.
Considerations of a primary melanoma on the skin, then, include how deep into the skin did it grow and whether it is ulcerated or not. That dictates how worried we are about it in terms of the risk that it could spread. We use these features to derive a stage for the melanoma, which in turn helps us understand what the likelihood is that the melanoma could come back somewhere else—in other words, spread somewhere else in the body. We can then have a discussion with an individual who’s facing melanoma about how high risk the melanoma is for coming back.
Substages of Stage II. We can further subdivide Stage II melanoma and think about substages this way:
The reason we are going over these substages is that adjuvant therapy, which we will be going over later, is currently FDA-approved only for Stages IIB and IIC melanoma.
As noted earlier, the staging system uses depth as one of the two key factors to distinguish between stages. For a more detailed discussion, you can see the sidebar, Staging Overview. The really simple way to think about invasive melanoma (melanoma that has penetrated into the dermis) is based on the following depths: less than 1 mm, 1 to 2 mm, 2 to 4 mm, and greater than 4 mm. An important difference here is noting that, when compared to other cancers where we talk about centimeters, with melanoma it’s millimeters. That is similar to a tiny amount of space between your two fingers.
I’ve mentioned invasive melanoma when discussing these depths, so we are talking about Stage I or Stage II melanoma here. There is also an additional melanoma stage called melanoma in situ, but that type of melanoma is not invasive—it is limited to the top layer of the skin (the dermis) and does not have a measurable depth.
Dr. Geoffrey Lim: And because we define how worried we should be based on millimeters, I use a common reference point to explain that to my patients, like 5-6 mm being roughly the diameter of a number two pencil eraser.
Dr. Jason Luke: Yes, that’s a helpful analogy, as shown in the diagrams. You can see how the melanoma depth generally increases with each substage of Stage II melanoma. The 3 substages of Stage II melanoma—IIA, IIB, and IIC—are shown in Graphics 1-3.
Stage IIA melanoma is more than 1 mm in depth but less than 2 mm and ulcerated (Graphic 1, left panel), or 2 to 4 mm in depth and not ulcerated (Graphic 1, right panel).
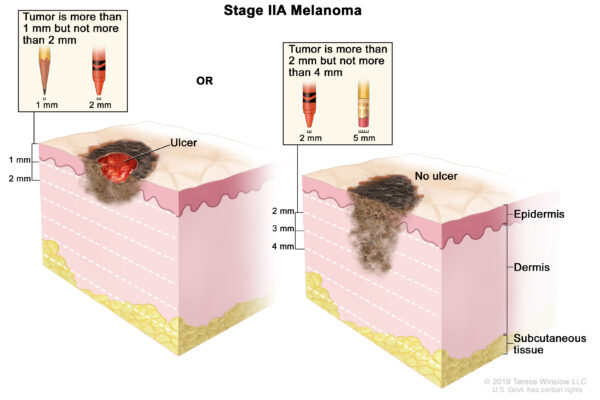
Graphic 1. Stage IIA melanoma. Figure adapted from Terese Winslow.
Stage IIB melanoma is 2 to 4 mm with ulceration (Graphic 2, left panel) or more than 4 mm and not ulcerated (Graphic 2, right panel).
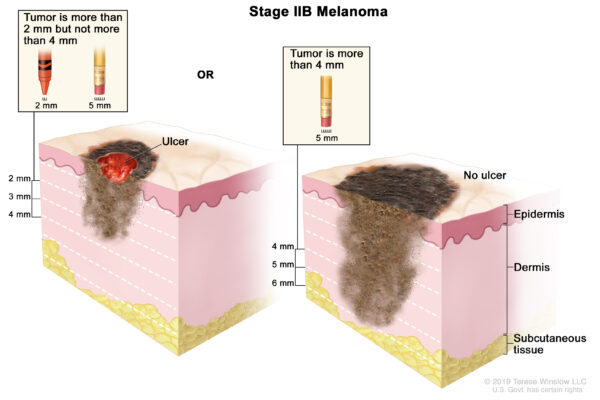
Graphic 2. Stage IIB melanoma. Figure adapted from Terese Winslow.
Stage IIC melanoma is more than 4 mm and ulcerated, as represented by the red depression in the center of the melanoma (Graphic 3).
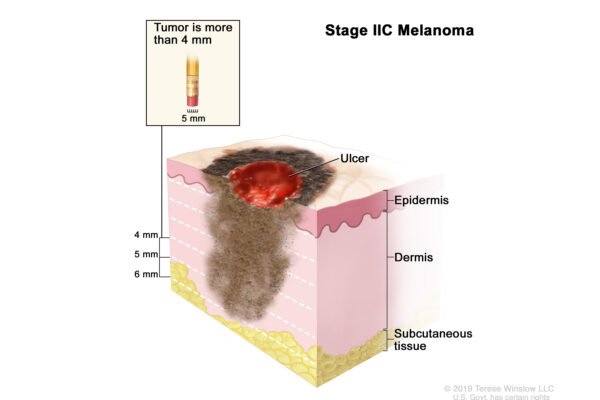
Graphic 3. Stage IIC melanoma: ulcerated and more than 4 in depth. Figure adapted from Terese Winslow.
For additional information about Stage II melanoma, click here.
Suggested Reading
Gershenwald JE, Scolyer RA, Hess KR, et al. Melanoma staging: Evidence-based changes in the American Joint Committee on Cancer eighth edition cancer staging manual. CA Cancer J Clin. 2017;67(6):474-492.